A 72 y/o man with hx of chronic alcoholism and smoking presents to your office with extreme fatigue. Denies any fever or weightloss or nightsweats. Vital signs were normal and physical examination reveals generalized small lymphadenopathy and mild splenomegaly. Laboratory studies reveal CBC with hgb 9.5, wbc 10k with 25% neutrophils, 65% mature lymphocytes and 9% monocytes, platelets 90k. LDH is increased at 600 and reticulocyte count of 8.0% . Haptoglobin level is 22mg% ( N 27 to 160) and urinary hemosiderin level is with in normal limits. Basic metabolic panel, Vitmain B12 and Folic acid levels are within normal limits. Peripheral smear is shown below and reveals many Smudge cells.
Most likely etiology of this patient’s Anemia is :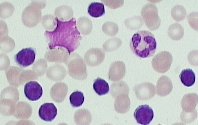
A. Microangiopathic Hemolysis
B. Bone marrow infiltration with Chronic Lymphocytic Leukemia
C. Acute Lymphoblastic Leukemia
D. Autoimmune Hemolysis
E. Hypersplenism
Copy Rights: USMLEGalaxy




I think it is d
i think B
answer autoimune Hemolysis D
b
Answer d Patient has Anemia associated with CLL.
B
D
D
D, CLL is associated with Autoimmune Hel=molytic Anemia and with immune thrombocytopenia, must treat with splenectomy and steroids…
hi from the explanation in question 4 it could be due t hemolysis or due to BM infiltration so which is more likely in this case?
thanks
E – hypersplenism
if it were intravasc hemolysis, urinary hemosiderin would be high. Yes, the haptoglobin a low, but not so much. If the bone marrow were infiltrated, the retic count wouldnt be this high.
D.
a
d
DDDDDDDDDDDDDDDDDDDDDDDDDDDD
LDH is elevated. Ans is D
E
interesting question…so, what is ther right answer?:) Thanx
B)smudge cells..CLL
D or B
Please give answer
B
I think it is because of autoimmune hemolysis. His LDH is high, hapto is low and retics are high. retics being high rules out marrow infiltration.if it was hypersplenism he would have pancytopenia but clearly CLL is the main issue in this guy.
Could I ask what the definitive answer to this question is?
Thanks
its e
Dr Red please explain this answer
This is a wrong question because it is very unlikely for a patient to have a clear picture of CLL with smudge cells and have a retic count of 8% at the same time. CLL is a malignancy where 99% of the time, the marrow is involved and Hemolytic anemia although present can never have a retic count of 8% because the production is hampered! Dr Redd will not answer this question hehe 😉
That is the whole point of this question! To recognize when 99% of bm is occupied vs. when it is not. When you have a retic like this , CLL is likely involving very less of bone marrow and therefore, need not be treated based on anemia alone because the cause of this anemia is autoimmune hemolysis associated with CLL not CLL associated myelophthisis . You are thinking in the right direction, keep it up but continue reading to get the grasp!
Dr Archer, the reticulocyte production index is 0.8%. I posted a comment today. Please dont mind the over-simplification (it’s not for you and my professional colleagues. It is meant to appeal to a casual reader of this blog). I wish to know if you concur with my understanding of this case. I may be mistaken but I think that this patient has CLL with Bone Marrow infiltration
Dear Adnan, your comments are welcome and we appreciate the details you provide. Other students will benefit from the explanations as well.
In this particular case, it is important to differentiate between autoimmune hemolysis and bone marrow infiltration by CLL as a cause of Anemia. Both these factors are known to cause anemia in CLL. it is important to identify the etiology because treatment differs. AIHA is treated with steroids and does not need active treatment for CLL. Please remember that Stage 0/I CLL is treated by Observation alone. Indications to treat in CLL are Anemia ( from bone marrow infiltration by CLL not from Autommune hemolysis), Thrombocytopenia, massive lymphadenopathy and constitutional symptoms. In order to establish that Anemia is from bone marrow infiltration due to CLL, AIHA needs to be excluded. If AIHA is excluded, treating CLL will help the anemia. If AIHA is established, AIHA must be treated with steroids and other treatments before actually, treating the CLL.
Not every hemolytic anemia is not adequately compensated. If hemolysis is severe, compensation will not help to completely normalize hemoglobin. Therefore,in severe hemolysis and in severe bleeding, anemia develops even when the bone marrow reserve is good. This patient’s bone marrow reserve is excellent and that is why the reticulocyte count is very good with respect to the degree of anemia.
A smudge cell suggests CLL.
Reticulocyte production index is 0.8%. (In an anemic patient, following the reticulocyte count can be misleading because the results are a percentage of the number of red cells in the blood; Like it is important to do an iron study in anemia, it is also important to confirm that the bone marrow is not in failure and that the reticulocytes are not erroneously elevated). This is done by a simple formula – reticulocyte count x (Hct divided by 45) x 0.5. This patient has CLL Myelopthisic Anemia (Myelopthisis). A value below 1% suggests that there is a reticulocyte production failure. In the options, the most likely cause of marrow failure would be Bone Infiltration by leukemic cells (B)
What could explain a low haptoglobin?
A co-existing hemolytic anemia – this can explain a low haptoglobin. Autoimmune hemolysis is associated with CLL. This is a very likely cause of low haptoglobulin in this patient. Low reticulocyte index and low haptoglobin suggest co-existing marrow failure and intravascular hemolysis with or without background iron deficiency anemia in any patient who has CLL with bone infiltration. Without a co-existing cause of marrow suppression, we can’t diagnose Autoimmune Hemolytic Anemia. It can’t explain why the reticulocyte production index is low. To confirm autoimmune hemolysis, we need confirmation by Coombs test. This patient’s presentation is rich with multiple diagnostic/clinical findings and etiologies. We need to very objective to find out the most likely etiology.
Evans syndrome will also cause low haptoglobin and low platelet and will explain the isolated neutropenia. It is a condition in which Autoimmune hemolysis exists with immune mediated thrombocytopenia.
Smokers are prone to red cell hemolysis. This can be the etiology of a low haptoglobin.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2716233/
http://www.ncbi.nlm.nih.gov/pubmed/12867276
http://emedicine.medscape.com/article/955266-workup – Evan’s syndrome
Why is urine hemosiderin normal?
Peripheral Blood Smear (picture) in this patient shows hypochromic cells and microcytes suggesting iron deficiency anemia. (IDA) – Does this patient actually have IDA? We don’t know. What would be the source of IDA?GI Bleeding? We don’t know. In IDA, there is not enough Hb pigment in red cells. When the red cell is hemolyzed, serum haptoglobulin engages the released Hb, but there is not enough iron (or Hb) in the cells to form hemosiderin. Hemosiderin is below the threshold for detection in this patient. It can also be absent! This patient may be losing blood through GI route.
Note – IDA can’t explain hemolysis (low haptoglobulin) even if low reticulocyte index is usual for IDA.
How do I exclude the other options?
A) CR-MAHA – Cancer related Microangiopathic Hemolytic anemia. This is a paraneoplastic syndrome with Coomb’s negative hemolytic anemia with schistocytes and thrombocytopenia. The blood film picture shows helmet cells (schistocytes, a sign of microangiopathic hemolytic anemia) and this patient also has low haptoglobin and thrombocytopenia. Even though, this etiology does not explain neutropenia, I will not go for this diagnosis until I have done a Coomb’s test and ruled out Autoimmune Hemolytic anemia.
C) Acute Lymphoblastic leukemia – There is no lymphoblast cell in the blood film shown. The cells shown have a dense chromatin which is more characteristic of more mature lymphocytes. Lymphoblasts have a more dispersed and more ‘fainter’ chromatin. This is not the most likely diagnosis.
E) Hyperspleenism – this will cause high reticulocyte and normal haptoglobin. It is seen in drug induced hemolytic anemia.
My answer is B. Yes, there is co-existing hemolytic and probably, iron deficiency anemia, but further confirmation is mandatory in these and the rest of the options. In option B, confirmatory bone marrow biopsy is very useful but low reticulocyte production index and pancytopenia is very satisfactory evidence of marrow failure (without further tests). The elevated lymphocytes are not functional. Neutrophils are functional in CLL but they are low here. A low haptoglobin and schistocytes( in the blood film picture) suggest hemolytic anemia. But low reticulocyte index and pancytopenia are against typical findings in hemolytic anemia. It does not conventionally suggest a hemolytic anemia. (This will cause elevated reticulocyte index). This suggests to me that there is co-existing marrow failure and hemolytic anemia. But Marrow suppression is still the most likely etiology. Why? Someone might ask this question if hemolytic anemia and marrow suppression co-exist. Most importantly, if production failure and hemolysis co-exist, like in this case, both will cause anemia. Then why choose marrow suppression over the other? Why do we look for the most likely etiology? The reason is that that treating marrow failure or the most likely etiology will raise or stabilize the cytopenic cell count. Treating hemolytic anemia will achieve neither of these, in marrow failure. Anemia will be refractory.
SIDE TALK: Why is it important to identify the most likely etiology? We do not want to delay proper treatment in a medical emergency. It is not an acceptable practice. Time is of the essence. Why not treat all forms of anemia at the same time? Lol it is simple, we can give a bone marrow transplant and place the patient on steroids but we don’t want to do bone transplant if the most likely cause is hemolytic anemia or iron deficiency. That is why we look for the most likely etiology. Treating the most likely etiology saves lives, costs less, and makes things less miserable for patients. For example relaxation and Tylenol will not treat epidural hematoma or meningitis. Delay is not acceptable in these scenarios. Even if you wish to start palliative care in a terminally ill patient, still, treating the most likely etiology has the same overwhelming benefits. This is the standard of care and looking for it is absolutely essential.
In this patient, as etiology, production failure takes priority because treating hemolysis first will not stop the cell count from falling (there are no new red cells)but treating the production failure can stop the red cell count from dropping (there are new red cells to replace the hemolyzing cells). Something that is destroying red cells will not cause anemia unless the capacity of the marrow to replace dying cells is exceeded. This can happen in both hemolytic anemia and marrow suppression. In this patient, there is evidence of marrow failure. The most likely etiology of anemia in this patient is pancytopenic marrow suppression. Treating every other etiology will be treatment failure. Even if we are enthusiastic to treat hemolysis, anemia will be refractory (and will get worse). A similitude to our treatment of this etiology will be like pouring cement or sand into a bag, on the bottom of which, there is a gaping hole. (Marrow failure is progressive; you don’t expect it to buy you any time if you start treating hemolytic anemia first).
Rectifications:
In severe hemolysis reticulocyte count may not be adequately compensated. Marrow response may be lagging behind.
Reticulocyte count given in this question has already been corrected for anemia. Even if it is not, RPI can be low in severe hemolysis.
Low haptoglobulin, high LDH, high reticulocyte count point more objectively towards hemolytic anemia. AIHA is the most likely contender for this form of anemia in CLL and it must be excluded first.
Low RPI in not diagnostic of bone infiltration. It is non specific. FDG PET scan or trephine biopsies are needed to diagnose bone infiltration.
Thank you Dr Archer.
RPI in this case is 2.5% which mean adequate bone marrow response
You’re correct. But I thought the question was a trick question and I thought 8% was a typing mistake (for 0.8%).
I held on to Sludge cells and throw my dart at Option B.
Apparently, CLL must not always have low RPI and it can present with high reticulocyte count when it co-exists with Autoimmune Hemolytic Anemia. I stand corrected. (please read my response to Alemieneh)
It was my earlier understanding that low reticulocyte production index (RPI) signifies Bone marrow failure. But I realized that marrow failure are of two types. One that is persistently low RPI and one that is initially low RPI. The latter occurs when the marrow is lagging behind in responsiveness but it will respond. There is variability of the erythropoeitic response in Autoimmune Hemolytic anemia. In the initial stage, RPI can be low. Autoimmune hemolytic anemia actually responds to glucocorticoids. In a study on 109 patients with Autoimmune hemolytic anemia, 15% had low RPI. http://www.ncbi.nlm.nih.gov/pubmed/3814817
(pls review this article)
Why this is not CLL marrow infiltrate?
Answer: Low RPI is not diagnostic of CLL ‘marrow infiltration’. For the diagnosis of CLL marrow infiltration, we need to do 18F FDG Pet scan or trephine biopsies. So this presentation is inconclusive for Marrow infiltration.
(Neutropenia and low platelet count can occur in Evan’s syndrome which is when Autoimmune hemolysis and Immune thrombocytopenia coexist.)
On the other hand, findings like high LDH, low haptoglobin are very highly suggestive features of hemolytic anemia. Autoimmune Hemolytic anemia (AIHA)has an association with CLL. Hemolysis can also occur in G6PD, SCD, or beta- thalassemia. These are insufficiently supported by the presentation and moreover, they are not in the list of options.AIHA occured in 4.3% of CLL patients in a single institutional study.
A low RPI can mean persistent marrow suppression, like in CLL marrow infiltration OR it could mean transient marrow suppression, like in Autoimmune hemolytic anemia. But why is this not CLL marrow suppression?
We can not conclude CLL (permanent marrow suppression) without excluding transient causes like hemolytic anemias, Iron deficiency. There is evidence of hemolysis in this question, and also some features of iron deficiency or anemia of chronic deficiency (microcytosis, hypochromia in the peripheral blood film)
Another reason, diagnostic tests for CLL marrow infiltration are not given (PET scan or trephine biopsies)
How can this be persistent marrow suppression without excluding transient suppression either by tests or supplementation.
The question has reticulocyte count of 8% but Adnan u keep on saying 0.8% didnt u see the question clearly or u are saying 8% reticulocyte is impossible in such cases ? if so why do u choose 0.8% specificaly? I am confused.
I am confusing reticulocyte count and reticulocyte production index.disregard my comment.
Click to access Xtra_online_reticulocytes.pdf
http://en.wikipedia.org/wiki/Reticulocyte_index
Alemieneh, please read the above link if you have the time otherwise just read on;
Reticulocyte count, Reticulocyte Index, Reticulocyte Production Index.
Reticulocyte count – reticulocytes as percentage of red blood cells – gives false high readings in anemia.
Reticulocyte Index – reticulocytes as percentage of hematocrit(or Hb) ratio – corrects for fluctuations in hematocrit ratio that will give false high or low reticulocyte readings.
Reticulocyte Production Index (most accurate) – corrects even for age of reticulocyte – reticulocytes as percentage of hematocrit ratio x maturation factor coefficient.
Hematocrit ratio – measured hematocrit (or Hb) divided by normal hematocrit or Hb. (usually normal hematocrit is taken as 45 for calculations) – read my previous posts for details.
SUMMARY:
Alemieneh, please don’t be confused. Initially I agreed with Muffadal. This question sounded impossible. A high reticulocyte count with smudge cells means that the Marrow is infiltrated by CLL cells (aka cancer) but how can marrow function be ‘super-excellent’ (Ret = 8%) in CLL. It sounded like a trick question. (like Dr Muffadal suggested)
I thought 8% was a typing error (for 0.8%). I thought that there was hard evidence of CLL (Sludge cells) but the only way this could be CLL was if the RPI, reticulocyte production index and/ or the reticulocyte count would be 0.8% (low) but Dr Archer corrected me.
Here goes:
In this question I learnt not to distrust the question, no matter how tempting it may sound.This is Autoimmune Hemolytic anemia (AIHA). Patient also has background CLL. This is a management issue.
CLL and AIHA are managed differently. We need to be sure we are managing the right thing. How do we know which is which?
A high Reticulocyte count suggests marrow function is ok so this is much more likely AIHA. (Option D)
Sorry for the confusion.
LEARNING POINT:
CLL can present with normal red cell production function.
CLL can co-exist with Autoimmune hemolytic anemia
We have to know the aetiology to treat the right disease.
Reticulocyte count (corrected) helps us to decide when to treat for CLL or AIHA. (low – CLL, high – AIHA)
Why coombs negative here ? It is autoimmunhemolytic anemua
D
B