Posted on February 28, 2012 by Archer USMLE Reviews
330) A 55 year old man is brought by the EMS to the emergency room in a disoriented state. The patient has alcohol smell on his breath. Reviews of his past records reveal history of chronic alcohol abuse. His girlfriend arrives in the ER few minutes later and she reports that the patient has not been eating anything because he has been drinking heavily and vomiting over the past three days. On examination, he is afebrile, blood pressure 130/82 mm Hg, RR 18/min and Pulse 82/min. When the nurse attempts to check blood pressure, the patient develops carpo-pedal spasm (Trousseau sign). Chest is clear to auscultation.
Laboratory investigations reveal:
Ethanol level 140mg%
Serum Sodium 142 meq/L
Serum Potassium 3.2meq/L
Serum Chloride 106meq/L
Calcium 6.2 mg% (N = 9.0 to 10.5)
Bicarbonate 25 meq/L
Creatinine 1.2 mg%
Albumin 3.9 gm% (N = 3.5 to 5.0 gm %)
Patient is treated with Calcium gluconate and then, another dose of calcium chloride. Repeat serum calcium level is 5.8mg%. Trousseau sign is still positive.
Which of the following is the most appropriate next step in managing this patient?
A) Obtain Serum Ionized Calcium
B) Obtain Serum Magnesium Level
C) Obtain Paratharmone level
D) Start potassium chloride
E) Obtain Vitamin D level
Filed under: Uncategorized, USMLE Test Prep | Tagged: ARCHER FLUID AND ELECTROLYTES, ARCHER NEPHROLOGY, dr.red nephrology lecture, usmle step 3 nephrology | 10 Comments »
Posted on February 28, 2012 by Archer USMLE Reviews
329) A 62 year old man presents to your office complaining of dry cough for past several months. Recently, he also noticed shortness of breath on exertion. He denies any fever, hemoptysis or weight loss. He has no history of infections. He does not smoke. He worked as a soft-ware consultant for past 40 years. He has no other medical problems and has never been hospitalized. On examination, he is afebrile, blood pressure 120/80 mm Hg, RR 18/min and Pulse 82/min. There are no palpable chest-wall masses or lymphadenopathy. On auscultation, fine crackles are heard at bilateral lung bases. A high resolution CT scan of the lungs shows sub-pleural cyst formation with honey combing. The patient undergoes an open lung biopsy for confirmation of diagnosis. Which of the following histo-pathological patterns is likely to be found in this condition?
A) Non-specific Interstitial Pneumonia ( NSIP)
B) Desquamative Interstitial Pneumonia (DIP)
C) Usual Interstitial Pneumonia (UIP)
D) Bronchiolitis Obliterans Organizing Pneumonia (BOOP)
E) Acute Interstitial Pneumonia (AIP)
Filed under: Uncategorized, USMLE Test Prep | Tagged: Archer pulmonology, archer step 3 pulmonology, USMLE STEP 3 PULMONOLOGY, usmle-step-3-pulmoology | 11 Comments »
Posted on February 28, 2012 by Archer USMLE Reviews
328) A 66 year old man is seen in your office for progressive shortness of breath on exertion for the past one year. He also reports dry cough. He denies any fever, hemoptysis or weight loss. He has no history of infections. He denies smoking. He has no other medical problems and has never been hospitalized. On examination, he is afebrile, blood pressure 120/80 mm Hg, RR 18/min and Pulse 82/min. There are no palpable chest-wall masses or lymphadenopathy. On auscultation, crackles are heard all over the lung fields, more pronounced at lung bases. Extremities show mild digital clubbing.
A chest x-ray is shown below:

Which of the following is expected to be seen with this disease?
A) Young age at onset
B) Rapid progression
C) High Resolution CT scans showing ill-defined cysts and pleural plaques
D) Poor or no response to steroids
E) Obstructive pattern on Pulmonary function tests
Filed under: Uncategorized, USMLE Test Prep | Tagged: Archer pulmonology, archer step 3 pulmonology, USMLE STEP 3 PULMONOLOGY, usmle-step-3-pulmoology | 16 Comments »
Posted on February 28, 2012 by Archer USMLE Reviews
327) A 16 year old boy presents to your office for a Pre-participation sports physical examination. He is healthy and physically active and has no complaints. He has no chest pain or shortness of breath. He denies any drug use or smoking. His maternal grandfather recently died suddenly of cardiac arrest from severe Myocardial Infarction at age 82. On physical examination, he is afebrile, pulse 82/min, Respiratory rate 18/min and blood pressure 106/76 mm Hg. Chest is clear to auscultation. Cardiac examination reveals a mid-systolic murmur, grade 2/6 heard best along the left sternal border. The murmur decreases in intensity when he stands and increases when he is supine. S1 and S2 are normal. The second heart sound is physiologically split. Cardiac impulse and carotid pulses are normal. The most appropriate action at this time:
A) Clear the patient for Sports participation
B) Refer to cardiology
C) Obtain 2D-Echocardiogram
D) Schedule Exercise Stress Test
E) Obtain Complete blood count
Filed under: Uncategorized, USMLE Test Prep | Tagged: Archer cardiology, archer pediatrics, archer sports medicine, USMLE STEP 3 CARDIOLOGY, usmle step 3 sports medicine, USMLE STEP3 PEDIATRICS | 19 Comments »
Posted on February 27, 2012 by Archer USMLE Reviews
326) A 55 year old african-american man presents to your office with complaints of shortness of breath that has slowly progressed over the past several months. He also reports chest pain which in non-pleuritic in nature. He has lost about 10lbs weight in the past three months. He has changed several jobs but he currently works as a sales representative for a drug company. On examination, his temperature is 100F, Pulse 98/min, RR 20/min and Blood Pressure 100/60 mm HG. He is in mild distress due to shortness of breath. On chest examination, there is dullness to percussion over the right side of the chest. No masses are palpable. Laboratory investigations reveal WBC 8k/μl with normal differential, Hgb 10.5gm%, Platelets 550k/μl, Calcium 11.2gm% ( (Normal 8.9 to 10.5 mg%)
A chest-x-ray is shown below:

Which of the following element in the history would be most helpful in making a presumptive diagnosis of his presentation?
A) Smoking
B) Family history of Cancer
C) Bone pain
D) Flank pain and Hematuria
E) Previous Occupation
Filed under: Uncategorized, USMLE Test Prep | Tagged: Archer pulmonology, archer step 3 pulmonology, USMLE STEP 3 PULMONOLOGY | 11 Comments »
Posted on February 26, 2012 by Archer USMLE Reviews
325 ) A 87 year old Caucasian man is evaluated in your office for progressive hearing loss. He reports defective hearing on both sides that started more than a year ago and has gradually worsened. The problem is particularly worse when he is in a crowded or noisy environment. He also reports frequent occurrence of roaring sounds and sounds similar to “ringing bells” in his ears. On otoscopic examination, he has mild cerumen impaction in bilateral ears. The Tympanic membranes are intact. Which of the following is the most characteristic feature seen with this condition?
A) Inability to hear “Vowel” sounds in the speech
B) Audiogram showing bilateral high-frequency sensory-neural hearing loss
C) Weber Test showing lateralization towards Right ear
D) A negative Rinne test
E) Otosclerosis
Filed under: Uncategorized, USMLE Test Prep | Tagged: Archer ENT, aRCHER GERIATRICS, audiometry evaluation, deafness, ear nose throat dosorders, ENT MCQs, geritrics mcqs, hearing loss, usmle ent mcq, USMLE STEP 3 ENT, usmle step 3 geriatrics, weber and rinne tests | 12 Comments »
Posted on February 26, 2012 by Archer USMLE Reviews
324) A 45 year old woman with history of Rheumatoid Arthritis presents to the emergency room increasing pain and swelling in her joints. She reports progressively increasing pain and stiffness of her bilateral wrist joints over the past two weeks. She now developed rapidly increasing pain and swelling in her right knee which prompted this Emergency Room visit. Her medications include Ibuprofen and Methotrexate. On examination, she is afebrile. There is mild swelling and tenderness in bilateral wrist joints. Right knee is warm, swollen and tender. Flexion and extension of the right knee are severely painful. Laboratory investigations are as follows:
WBC 9.0k/µl
Differential: Neutrophils 65%, Lymphocytes 24%, Monocytes 7%
Hemoglobin 11.5 g/dL ( Normal = 13.0 to 16.5 gm%),
Mean cell volume (MCV) 84 fL
Platelet count 510k/µl ( Normal 180 to 350k⁄μl )
ESR : 70 mm/hr
Which of the following is the most appropriate next step in management?
A) Pulse Methyl Prednisolone
B) Oral Prednsione
C) Arthrocentesis
D) Discontinue Methotrexate and start Infliximab
E) Intra-articular Glucocorticoids
Filed under: Uncategorized, USMLE Test Prep | Tagged: Archer Rheumatology, Rheumatoid arthritis, USMLE step 3 Rheumatology | 9 Comments »
Posted on February 26, 2012 by Archer USMLE Reviews
323) A 65 year old man is evaluated in your office for slowly progressing involuntary shaking movements in his hands. He noticed these movements about 10 months ago which have slightly worsened now. Occasionally, he was told by his wife that his head shakes as well. The movements have led him to feel socially embarrassed because they are worse when he attempts to write or hold a cup of coffee or fasten a shirt button. He denies any tremors in his legs. He denies any problems with his gait or muscle pain or stiffness. He reports drinking wine on daily basis since the tremors have started because he thinks alcohol appears to improve the tremors. He denies using any medications. There is no family history of tremors or seizures. On examination, he appears comfortable. Tremors are visible bilaterally with his arms outstretched and they are increased when asked to hold a cup filled with water. His handwriting is large and tremulous. Gait is normal with normal arm-swing. There are no other neurological deficits. Routine chemistry panels including TSH and Liver function tests are normal. Which of the following is the most appropriate next step in management?
A) MRI brain with contrast
B) Vitamin B12 level
C) Trial of Dopamine Agonist
D) Initiate Propranolol Therapy
E) Serum Cerulopalsmin level
F) Start oral Primidone
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer neurology, neurology mcqs, neurology usmle mcqs, parkinson tremor, usmle step 3 neurology | 13 Comments »
Posted on February 26, 2012 by Archer USMLE Reviews
322) A 45 year man is evaluated in emergency department for severe cough accompanied by bloody expectoration. Cough is of 4 month duration associated with sputum production but he is worried because of the new change in the character of his sputum which is now frankly bloody. He reports a weight-loss of 10 lbs in the past two months. He has intermittent nigh-sweats and low grade fever on a daily basis. On examination, his temperature is 100F, Pulse 98/min, RR 20/min and Blood Pressure 100/60 mm HG. He appears cachectic and in moderate distress due to cough. On auscultation, high-pitched bronchial breath sounds are heard in the right upper chest.
A chest-x-ray is shown below:

The patient is admitted and is placed on respiratory, negative-pressure isolation. HIV rapid test is positive. Sputum smears for Acid Fast Bacilli (AFB) are positive. A CD4 count is 155/μl ( Normal = 650 to 1150/µl). Which of the following is the most appropriate next step in management at this time?
A) Bronchoscopy and send bronchial washing for clutures
B) Start Multi-Drug anti-tuberculosis Therapy alone
C) Start Highly Active Antiretroviral Therapy (HAART) plus Multi-drug Anti-TB therapy
D) Start HAART and await sputum for AFB identification and sensitivity testing
E) Start Clarithromycin for Mycobacterium Avium Intracellulare (MAC)
Filed under: Uncategorized, USMLE Test Prep | Tagged: Archer Infectious Diseases, Archer pulmonology, USMLE STEP 3 INFECTIOUS DISEASES, USMLE STEP 3 PULMONOLOGY | 39 Comments »
Posted on February 7, 2012 by Archer USMLE Reviews
321) A 45 – year-old obese woman presents to your office complaining of a skin lesion on her left shin. This lesion started spontaneously 3 weeks ago and appeared like a small bruise. Over the past two weeks, the lesion has enlarged and the overlying skin has become hardened and raised with reddish border. There is no pain or itching. She denies any recent trauma. She lives in Texas but one month ago, she traveled to New England region to visit a friend. She is sexually active with one partner and occasionally, uses condoms.. Her past medical history is unremarkable. On physical examination, there is an oval shaped lesion on her left shin. The border is indurated and red in color with yellowish, atrophic appearance in the center. An image of the lesion is shown below:
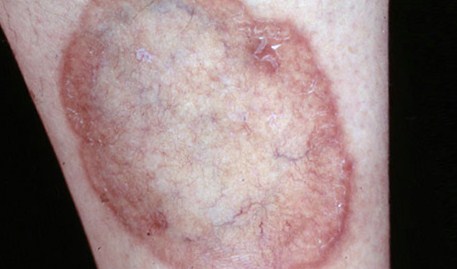
Which of the following investigations should be ordered next?
A) Lyme serology
B) Hemoglobin A1C
C) Anti-Myeloperoxidase ( P-ANCA)
D) Colonoscopy
E) Herpes Simplex Virus (HSV) Serology
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, dermatology usmle, dermatology usmle step 3 questions, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images | 22 Comments »
Posted on February 7, 2012 by Archer USMLE Reviews
320) A 65 – year-old woman is evaluated in your office during a follow-up visit. Her medical problems include Diabetes mellitus type II and hypertension. She is being managed on oral metformin, glyburide and hydrochlorthiazide. Her most recent hemoglobin A1C is 6.5%. Her urine was negative for microalbumin three months ago. Her past medical history is significant for hospitalization for angioedema which occured after initiation of Enalapril three years ago. Physical examination is unremarkable. The patient requests if she can be started on Angiotensin Receptor Blocker ( ARB) because she read about its beneficial effects in preventing kidney damage in diabetics. Which of the following is the most appropriate response?
A) “You are correct. I will start you on ARB”
B) ” You can not be started on ARB because of history of Angioedema”
C) “You can start ARB but need pre-medication with steroids”
D) ” You can start ARB but there is a small risk of Angioedema”
E) ” Hydralazine/ Nitrate combination offers similar reno-protective effect as ARB”
Filed under: Uncategorized, USMLE Test Prep | Tagged: Archer cardiology, ARCHER NEPHROLOGY, dr.red nephrology lecture, USMLE STEP 3 CARDIOLOGY, usmle step 3 nephrology | 9 Comments »
Posted on February 7, 2012 by Archer USMLE Reviews
319) A 64-year-old man with history of diabetes mellitus and end-stage renal disease is admitted for complaints of weakness and contractures in his extremities associated with tight and thickened skin. He denies any past history of finger or toe discoloration on exposure to cold. He is dialysis dependent and undergoes hemodialysis three times in a week. His most recent dialysis was a day ago. His symptoms started 3 days prior to presentation and have progressively worsened. Three weeks prior to admission , the patient had a transient ischemic attack. An MRI with Gadolinium performed at that time did not reveal any abnormalities. He denies any neurological symptoms at this time. The patient’s medications upon admission include Aspirin, Insulin Glargine and Lisinopril. On physical examination, the patient appears chronically ill. He is afebrile, blood pressure 120/70 mmHg and pulse rate was 82/minute. Skin examination reveals diffuse nonerythematous thickening and tightening of the skin over the abdomen, arms and legs. Chest and the face are spared. There are contractures in upper and lower extremities extremely limiting the range of motion of the involved joints. Erythrocyte sedimentation rate and C-reactive protein are elevated. Calcium is 8.0mg% and phosphorous 4mg% with calcium – phosphorous product of 32. An image of his upper extremity is shown below

Which of the following is the most likely diagnosis?
A) Systemic sclerosis
B) Calciphylaxis
C) Nephrogenic Systemic Fibrosis
D) Cryoglobulinemia
E) Eosinophilc Fascitis
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, ARCHER NEPHROLOGY, dermatology usmle, dermatology usmle step 3 questions, dr.red nephrology lecture, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images, usmle step 3 nephrology | 10 Comments »








