Posted on November 15, 2015 by Archer USMLE Reviews
479. A 57 year old female presents for second opinion of a left breast lesion that had been diagnosed as ‘eczema’ by her regular nurse practitioner, which briefly improved after a short course of topical steroids. On physical exam there is an erythematous, scaly lesion involving the left breast. Image is shown below. Her last mammogram was a year ago and it was “fine”. She does not report any family history of breast cancer. What is the next step in the patient’s management?

A – Bilateral breast ultrasound
B – Bilateral mammography and punch biopsy of nipple
C – Maintain regular annual mammography appointment
D – Oral corticosteroids
E – Left breast MRI
Filed under: USMLE STEP III QUESTION BANK, USMLE Test Prep | Tagged: archer dermatology, archer general internal medicine, Archer Gynecology, internal medicine board review, USMLE STEP 3 DERMATOLOGY, usmle step 3 gynecology | 18 Comments »
Posted on September 14, 2015 by Archer USMLE Reviews
A 2-week-old infant is brought to the office for a regular postnatal follow-up. She was born after an uneventful term pregnancy to a 29-year-old G2P2 woman. Mother reports that the infant is feeding well and seems active. No evidence of any fever. The parents are worried about the ‘rash’ that appeared over the infant’s left cheek. On examination, a lesion is noted on the infant’s left cheek as shown below. Vital signs are within normal limits. What is the most appropriate next step in management of this finding?

| A |
Surgical excision of the entire lesion |
| B |
Biopsy of the lesion |
| C |
Laser removal of the lesion |
| D |
Reassurance and observation |
| E |
Topical 5-fluoro-uracil |
Filed under: USMLE STEP III QUESTION BANK, USMLE Test Prep | Tagged: archer dermatology, archer pediatrics, dermatology usmle, dermatology usmle step 3 questions, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images, usmle step 3 pediatrics | 9 Comments »
Posted on May 7, 2012 by Archer USMLE Reviews
424) A 3 day old male infant is evaluated for a rash that developed previous night and has been progressing. The rash first started on his face as flat red patches but now it has become bumpy and some of them have pus in it. The baby is breast feeding and there is no history of fever. The mother is healthy and none of the family members are sick at home. The baby was born by an uncomplicated vaginal delivery. On examination, he is afebrile. There are numerous small flat red patches along with yellowish-white papules and numerous pustules all over his trunk and extremities. The lesions on his face seem to be resolving. Palms and soles are not involved. A Wright-stained smear of pustular fluid shows numerous eosinophils and occasional neutrophils. A picture of the rash is shown below:

Which of the following is the most likely diagnosis?
A) Miliaria
B) Eosinophilic Pustular Folliculitis
C) Erythema Toxicum
D) Milia
E) Staphylococcal Pyoderma
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, archer pediatrics, usmle step 3 dermatology images, usmle step 3 pediatrics | 10 Comments »
Posted on May 7, 2012 by Archer USMLE Reviews
423) A 14 month old male baby is brought to your office by his concerned mother for recurrent diarrhea over the past 2 months. He also developed a scaly rash around his mouth, on the cheeks and on buttocks. He has been exclusively breast-fed for about 8 months and has been started on gradual weaning process over the last four months. He is otherwise, a healthy child. There is no family history of eczema. On examination, he is afebrile and vitals are stable. Physical examination shows lesions around the ano-genital area as shown below :
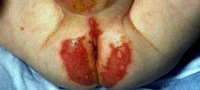
Similar lesions are seen over his cheeks and around the mouth. Which of the following is indicated in this patient at this time?
A) Exclusive Breastfeeding
B) Serum Lead level
C) Serum Zinc level
D) Glucoagon level
E) Sweat Chloride Level
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, archer pediatrics, usmle step 3 dermatology images, usmle step 3 pediatrics | 10 Comments »
Posted on February 7, 2012 by Archer USMLE Reviews
321) A 45 – year-old obese woman presents to your office complaining of a skin lesion on her left shin. This lesion started spontaneously 3 weeks ago and appeared like a small bruise. Over the past two weeks, the lesion has enlarged and the overlying skin has become hardened and raised with reddish border. There is no pain or itching. She denies any recent trauma. She lives in Texas but one month ago, she traveled to New England region to visit a friend. She is sexually active with one partner and occasionally, uses condoms.. Her past medical history is unremarkable. On physical examination, there is an oval shaped lesion on her left shin. The border is indurated and red in color with yellowish, atrophic appearance in the center. An image of the lesion is shown below:
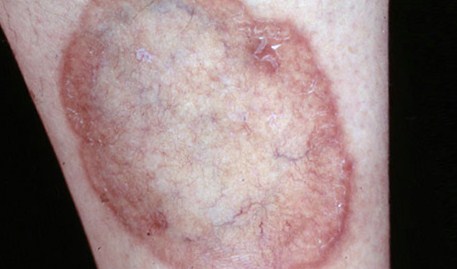
Which of the following investigations should be ordered next?
A) Lyme serology
B) Hemoglobin A1C
C) Anti-Myeloperoxidase ( P-ANCA)
D) Colonoscopy
E) Herpes Simplex Virus (HSV) Serology
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, dermatology usmle, dermatology usmle step 3 questions, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images | 22 Comments »
Posted on February 7, 2012 by Archer USMLE Reviews
319) A 64-year-old man with history of diabetes mellitus and end-stage renal disease is admitted for complaints of weakness and contractures in his extremities associated with tight and thickened skin. He denies any past history of finger or toe discoloration on exposure to cold. He is dialysis dependent and undergoes hemodialysis three times in a week. His most recent dialysis was a day ago. His symptoms started 3 days prior to presentation and have progressively worsened. Three weeks prior to admission , the patient had a transient ischemic attack. An MRI with Gadolinium performed at that time did not reveal any abnormalities. He denies any neurological symptoms at this time. The patient’s medications upon admission include Aspirin, Insulin Glargine and Lisinopril. On physical examination, the patient appears chronically ill. He is afebrile, blood pressure 120/70 mmHg and pulse rate was 82/minute. Skin examination reveals diffuse nonerythematous thickening and tightening of the skin over the abdomen, arms and legs. Chest and the face are spared. There are contractures in upper and lower extremities extremely limiting the range of motion of the involved joints. Erythrocyte sedimentation rate and C-reactive protein are elevated. Calcium is 8.0mg% and phosphorous 4mg% with calcium – phosphorous product of 32. An image of his upper extremity is shown below

Which of the following is the most likely diagnosis?
A) Systemic sclerosis
B) Calciphylaxis
C) Nephrogenic Systemic Fibrosis
D) Cryoglobulinemia
E) Eosinophilc Fascitis
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, ARCHER NEPHROLOGY, dermatology usmle, dermatology usmle step 3 questions, dr.red nephrology lecture, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images, usmle step 3 nephrology | 10 Comments »
Posted on December 30, 2011 by Archer USMLE Reviews
296) A 6 month old Asian infant is brought by his concerned aunt for evaluation of dark blue areas on the child’s buttocks. She says she was called to baby-sit the infant since his mother found a new job 2 days ago. She noted the rash and became suspicious that the child may have been abused. The mother arrives in Emergency room an hour later and reports that the rash has been present since birth. The mother is divorced and lives alone with the child. On examination, there are bluish-green patches on bilateral buttocks and on the lower back. They are irregular in shape and margins are indistinct. There is no swelling or tenderness. An image of the skin findings is shown below:

Which of the following is the most appropriate next step ?
A) Order Skeletal Survey
B) Reassure that rash may fade away in few years
C) Contact Child Protection services
D) Obtain Coagulation parameters
E) Obtain Platelet count
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, archer pediatrics, dermatology usmle, dermatology usmle step 3 questions, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images, USMLE STEP3 PEDIATRICS | 10 Comments »
Posted on December 30, 2011 by Archer USMLE Reviews
295) A 10 year old boy is brought to your office for evaluation of rash in bilateral axillae and groin for the past 2 months. He denies any itching or any other skin rashes. However, he reports that the area has become progressively rough to touch. He is otherwise, healthy. On examination, there are reddish brown patches in bilateral axillae and groin. There is maceration and scaling in the web spaces between the toes of bilateral feet. Rest of the examination is normal. A KOH mount is obtained and is negative. Wood’s lamp examination reveals coral red fluorescence. A picture of the rash is shown below:

Which of the following is the most appropriate next step ?
A) Topical corticosteroid
B) Topical Selenium Sulfide
C) Oral erythromycin
D) Topical Clotrimazole
E) Oral Metronidazole
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, archer pediatrics, dermatology usmle, dermatology usmle step 3 questions, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images, USMLE STEP3 PEDIATRICS | 7 Comments »
Posted on August 21, 2011 by Archer USMLE Reviews
251 ) A 65 year old woman is evaluated in your office for pain in bilateral feet for the past four weeks. The pain is burning in quality and is associated with intense itching. Her past medical history is significant for difficult to control Type II Diabetes Mellitus. Her recent HgbA1C was 7.9% and Creatinine was 1.8mg%. On physical examination, she is obese, afebrile and in no apparent distress. She has diminished pinprick and vibration sensation in glove and stocking pattern in bilateral upper and lower extremities. Dorsalis pedis and posterior tibial pulses are mildly diminished. There are multiple erythematous tiny vesicles between the toes and on the plantar aspect of the both feet. Which of the following is the most appropriate treatment option for this patient’s pain?
A) Oral Pregabilin
B) Topical Corticosteroids
C) Oral Cefazolin
D) Topical Terbinafine
E) Topical Acyclovir
Filed under: USMLE Test Prep | Tagged: archer dermatology, Archer endocrinology, Archer Infectious Diseases, archer neurology, USMLE STEP 3 DERMATOLOGY, usmle step 3 endocrinology, USMLE STEP 3 INFECTIOUS DISEASES | 9 Comments »
Posted on August 9, 2011 by Archer USMLE Reviews
249 ) A 64 year old man is evaluated in your office for a left sided headache that started 24 hours ago. He describes the headache as a burning sensation over his left temple and the forehead. He also reports fatigue and malaise for the past one day. He has no significant past medical history. On examination, he has a low grade fever at 100.4F, Blood pressure is 120/70 mm Hg. Physical examination reveals hyperesthesia on his left forehead and skin findings as shown in the picture below:

Which of the following is the most appropriate immediate next step in management ?
A) Mupirocin cream
B) Start Oral Cephalexin
C) Refer to Ophthalmology
D) Refer to Dermatology
E) Topical Acyclovir
Filed under: USMLE Test Prep | Tagged: archer dermatology, Archer Infectious Diseases, dermatology usmle, dermatology usmle step 3 questions, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images, USMLE STEP 3 INFECTIOUS DISEASES | 11 Comments »
Posted on July 9, 2011 by Archer USMLE Reviews
227 ) A 32 year old man is evaluated in the clinic for intensely itchy rash . The rash appeared suddenly on his trunk 24 hours ago and has spread to his extremities. He denies any fever or using any recent medications. His travel history is significant for a trip to Colarado 3 days ago where he stayed with his friend in a hotel room. He enjoyed camping in the mountains and spent his evenings in the hotel building’s swimming pool. On examination, there are multiple red papules all over his body and extremities but not on the head and the neck. Some of the papules are tender. Which of the following is the most appropriate next step in management?
A) Doxycycline
B) Lyme Serology
C) Ciprofloxacin
D) Reassurance
E) Amoxicillin-Clavulunate
Filed under: USMLE Test Prep | Tagged: archer dermatology, Archer Infectious Diseases, archer pediatrics, archer preventive medicine, archer travel medicine, itchy traveler, travel medicine, USMLE STEP 3 DERMATOLOGY, USMLE STEP 3 INFECTIOUS DISEASES, usmle step 3 pediatrics, usmle step 3 preventive medicine, usmle step 3 travel medicine | 4 Comments »
Posted on June 26, 2011 by Archer USMLE Reviews
205) A 27 year old woman, primigravida at 35 week gestation is evaluated in your office for extreme itching associated with rash. The rash and itching first started on her abdomen but now spread to her buttocks and legs as well. She denies similar complaints in any of her family members. On physical examination, an eruption consisting of small erythematous wheals is noted mostly in the abdominal striae with sparing of the peri-umbilical skin. Some rash is also noted on her lower extremities. There is no involvement of palms and soles. A picture of her abdomen is shown below:

Most likely diagnosis:
A) Scabies
B) Pemphigoid Gestationis
C) Intahepatic Cholestasis of Pregnancy (ICP)
D) Pruritic Urticarial Papules of Pregnancy (PUPP)
E) Pruritic folliculitis of Pregnancy
Filed under: USMLE Test Prep | Tagged: archer dermatology, Archer Gynecology, archer obstetrics, archer ostetrics and gynecology, obstetrics, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images, usmle step 3 gynecology, usmle step 3 gynecology and obstetrics, usmle step 3 obstetrics | 5 Comments »
Posted on June 24, 2011 by Archer USMLE Reviews
193) A 22 year old woman is evaluated in the office for recurrent attacks of colicky abdominal pain that resolve spontaneously. During the episodes, the pain lasts about 8 to 10 hours and resolves spontaneously. Several clinical examinations, laboratory investigations and imaging studies in the past have failed to reveal any clear etiology. She also reports recurrent swelling of her hands and feet, the last episode being 2 weeks ago. Physical examination is benign. A complete blood count and comprehensive metabolic panel are with in normal limits. Which of the following is most helpful in confirming the suspected diagnosis?
a) Urinary Porphobilinogen
b) Radio Allergosorbent Test ( RAST)
c) Anti-nuclear antibodies
d) C1-Inhibitor
e) 24 hour delta-aminolevulinic acid
Filed under: USMLE Test Prep | Tagged: archer dermatology, ARCHER GASTROENTEROLOGY, USMLE STEP 3 DERMATOLOGY, USMLE STEP 3 GASTROENEROLOGY | 5 Comments »
Posted on June 24, 2011 by Archer USMLE Reviews
192) A 26-year-old man is evaluated for a history of recurrent headaches and palpitations for the past one month. At this time, he has no headache or palpitations. He denies any chest pain, dizziness or shortness of breath. His past history is unremarkable except for fleshy nodules over his trunk that have been present since adolescence and have been increasing in number. On physical examination, heart rate is 102/min; blood pressure is 168/100 (Lying) and 138/90 ( Standing). Skin examination reveals freckling in the inguinal region and several fleshy tumors on his back as shown in the picture:
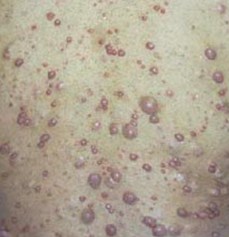
An Electrocardiogram reveals Sinus Tachycardia. The most appropriate next step in management of this patient?
a. Biopsy of the tumors
b. Plasma Metanephrines
c. CT Scan of the abdomen
d. Intravenous fluids
e. 24-Hour holter monitoring
Filed under: USMLE Test Prep | Tagged: Archer cardiology, archer dermatology, USMLE STEP 3 CARDIOLOGY, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images | 5 Comments »
Posted on June 14, 2011 by Archer USMLE Reviews
181) A 35 year-old man with history of ulcerative colitis is seen in your office for nodular, tender skin lesions on both of his anterior legs. He was diagnosed with ulcerative colitis about 6 months ago when he first presented with severe bloody diarrhea. He was initially managed with steroids and is now, being maintained on Mesalamine. A colonoscopy at the time of diagnosis revealed pancolitis. He has no diarrhea now. There is no evidence of weight-loss. Physical examination reveals tender erythematous lesions on the anterior aspect of his bilateral lower extremities. Laboratory investigations reveal leucocytosis and elevated C-reactive protein. Which of the following is a poor prognostic factor in Inflammatory Bowel Disease?
A) Proctitis
B) Erythema nodosum
C) Albumin of 4.1 gm/dl
D) Lymphocytosis
E) Elevated ANCA (anti-neutrophilic cytoplasmic antibodies) level.
Filed under: USMLE Test Prep | Tagged: archer dermatology, ARCHER GASTROENTEROLOGY, USMLE STEP 3 DERMATOLOGY, USMLE STEP 3 GASTROENEROLOGY | 4 Comments »
Posted on June 14, 2011 by Archer USMLE Reviews
Q180) A 35 year old woman presents with a 3-week history of nodular lesions on her lower legs. She states that he had similar lesions that appeared few years ago and spontaneously resolved . She denies any recent infection except for an upper respiratory infection for which he was treated with antibiotics 2 weeks ago. She is currently not on any medications. He denies any weightloss or diarrhea or constipation. She has no cough or night sweats. Physical examination revealed erythematous nodular swellings on the anterior lower legs. The lesions are tender to palpation.

–
The most common etiology of these lesions world-wide:
A) Tuberculosis
B) Inflammatory bowel disease
C) Sarcoidosis
D) Diabetes Mellitus
E) Streptococcal infection
F) Herpes Simplex Virus
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images, USMLE Step 3 question bank, usmle step 3 questions | 3 Comments »
Posted on June 14, 2011 by Archer USMLE Reviews
Q179) A 48 Year old woman is evaluated in your office for a skin eruption that appeared three days ago. Her past medical history is significant for Rheumatoid arthritis for which she uses Methotrexate. She recently had increasing joint pain and she was placed on ibuprofen which takes about three times daily. Her joint pain is well controlled now. She is now concerned about the skin eruption that is predominantly distributed on her arms, hands and feet. The eruption is painless. On examination, there is no joint swelling or tenderness, range of motion in the joints is normal. Skin examination reveals the lesions as shown in the image below.

The most appropriate management option for this patient:
A) Observation
B) Stop Ibuprofen
C) Start Acyclovir
D) Intra-lesional corticosteroids
E) Anti-citrullinated pep-tide levels
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images, USMLE Step 3 question bank, usmle step 3 questions | 4 Comments »
Posted on June 14, 2011 by Archer USMLE Reviews
Q177) A 55-year-old white woman is seen in your office for a 6-month history of slowly enlarging lesions on both lower extremities. She is otherwise healthy. The lesions are painless. She denies any trauma to these areas. Her past medical history is significant for diabetes mellitus diagnosed 2 years ago and rheumatoid arthritis. Her medications include Metformin, Enalapril and Methotrexate. On skin examination, she has 2 cm yellow, smooth, firm centrally depressed plaques involving the thighs and knees. Image is shown below

The most likely underlying etiology :
A) Drug-induced
B) Rheumatoid arthritis
C) Diabetes Mellitus
D) Malignancy
E) Sarcoidosis
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, Archer endocrinology, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images, USMLE Step 3 question bank, usmle step 3 questions | 3 Comments »
Posted on June 14, 2011 by Archer USMLE Reviews
Q177) A 52 Year old obese man is evaluated in your office during a routine annual visit. He denies any fatigue or recent weight changes. He has normal appetite and physically active. He had a colonoscopy 1 year ago that was normal. On physical examination, he is obese with a BMI of 34. Skin examination reveals the findings shown in the image below :

Which of the following is most likely to be seen in this patient?
A) Diabetes Mellitus, Type I
B) Gastric cancer
C) Increased Insulin levels
D) Hyperthyroidism
E) Addison’s disease
Filed under: Uncategorized, USMLE Test Prep | Tagged: archer dermatology, Archer endocrinology, Archer oncology, USMLE STEP 3 DERMATOLOGY, usmle step 3 dermatology images, USMLE Step 3 question bank, usmle step 3 questions | 4 Comments »


















